Reading an MRI report can be overwhelming. There are are a lot of big words, and you may not know what they all mean, but often they don't sound good. Have you ever found yourself wondering:
"What Does My MRI Report Mean?"
In this post, I'll explain some of the most common spinal MRI findings in plain, simple terms so that you can better understand your MRI report with out getting anxious or overwhelmed.

Understanding Spinal MRI Terminology
First, let's get some terminology out of the way.
Your lumbar spine or lower back has five vertebrae labeled from L1, L2, L3, L4, L5 from top to bottom.
The discs between them or the joints are named L1-L2 or L4-L5, etc. The very bottom one is L5-S1, with S1 signifying the first sacral vertebrae.
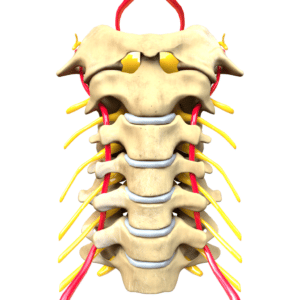
This is the naming convention, which also applies to the neck or the cervical spine.
There are seven vertebrae going from C1 to C7, with discs and joints named, for example, C3-C4 or C5-C6.
Degenerative Joint and Degenerative Disc Disease on MRI
Now, let's move on to degenerative changes in the spine.
These are common findings on MRI reports, especially in people over 40, but they can start earlier in life - as young as the 20s.
Degenerative Joint Disease (a.k.a. Spondylosis)
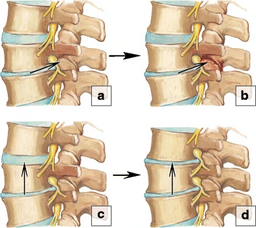
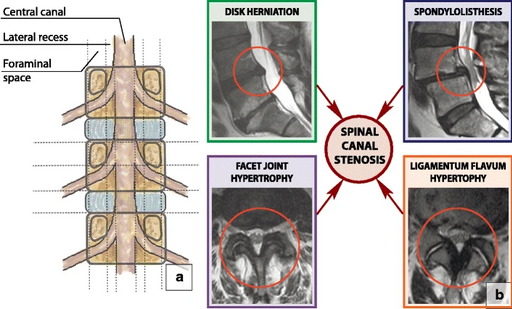
Degenerative joint disease (DJD) is a wearing down of the facet joints, as shown by the arrow in the top picture (b). Basically, it's another word for osteoarthritis.
Technically degenerative joint disease can occur in any joint in the body whereas spondylosis is a term that refers specifically to DJD in the spine.
Spondylosis can cause pain and irritation in the neck or back as the face joints get smashed together.
However, positioning can often help create more space between these facet joints. Bending forwards or away from the affected side opens up the spaces, while bending backward or towards the affected side narrows them.
Degenerative Disc Disease (DDD)
Degenerative disc disease (DDD) is a loss of disc height between the vertebrae. The spinal discs contain a lot of water, but as you age, your discs naturally dry out. That's why people tend to lose a few inches of height as they age.
However, some discs may lose more height than others. This usually happens in segments of the spine that are hypermobile (move too much).
This loss of disc height can also jam the facet joints together as well as narrow the openings (foramen) where the nerve roots exit the spine. This narrowing, known as foraminal stenosis, can cause pain, numbness, or tingling.
How common are these MRI findings?
These MRI findings are pretty common, even in people without pain. Below is a table from a 2015 systematic review in American Journal of Neuroradiology of image findings in assymptomatic people. For context, a systematic review combines the results of multiple other studies. It's considered to be the highest level of research evidence.
Source: W Brinjikji, et al. Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. Am J Neuroradiol. 2015; 36(4):811-6.
As you can see, disc degeneration on MRI is pretty common even in young people and becomes increasingly common with age.
Facet degeneration (DJD) on the other hand becomes more common after the age of 50 and also increases with age.
Spondylosis, Spondylolysis, and Spondylolisthesis on MRI
The terms spondylosis, spondylolysis, and spondylolisthesis can be confusing. "Spondy" is the latin root for "spine". The suffix of each of the words determines what the corresponding condition of the spine is.
Spondylosis
As noted above, this is basically just degenerative joint disease (arthritis) of the spine. The suffix -osis technically means "an abnormal condition of" or "disease of".
Spondylosis
Spondylolysis means a fracture in a part of the vertebrae called the pars interarticularis. (-lysis = "defect").
This type of fracture can happen from injury, but it can also happen gradually over time. Around 1 in 20 people develop these, so don't get extremely worried if you happen to see one on your MRI.
Spondylolisthesis
If you have had a spondylolysis as described above, the vertebra can start to slip forward on the one below it.
This slipping of the vertebrae known as spondylolisthesis. It may also be called anterolisthesis, meaning forward slipping. Spondylolisthesis is graded from 1 to 5.
Grades 4 and 5 are legitimately cause for concern, but if you have a Grade 1 or 2 spondylolisthesis on your MRI, there's probably no reason to immediately worry.
Retrolisthesis
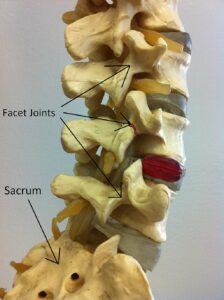
Retrolisthesis is the opposite of anterolisthesis, where a vertebra slips backward on the one below.
Here you can see a retrolisthesis of L5 slipping backward on S1.
If you have a spondylolisthesis on your MRI, don't get overly concerned, especially if you're over the age of 60.
In younger people, spondylolisthesis is usually a result of a pars fracture. However, as you age and lose water content in your discs (DDD), the discs become a little "looser" allowing your vertebrae to slide more.
That's why spondylolisthesis starts becoming more common after 60 years of age.
Spinal Stenosis on MRI
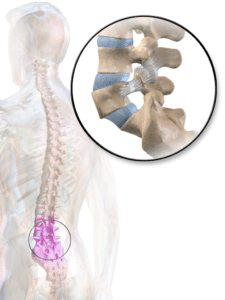
Spinal stenosis refers to the narrowing of spaces in the spine. This can occur either in the neck (cervical spinal stenosis) or in the lower back (lumbar spinal stenosis).
3 types of spinal stenosis you may see on your MRI
You can get steonsis "narrowing" of the central canal, the lateral recesses, or the foraminal spaces where nerve roots exit.
While not overly concerning if you only have back pain, symptoms like loss of bowel or bladder control, numbness, tingling, or weakness in the legs or arms warrant further investigation and treatment.
Bulging, Protruding, and Herniated Discs on MRI
Finally, vertebral disc dysfunction, including bulging, protrusion, extrusion (herniation), and sequestration is worrisome for a lot of people.
Many people worry about having a "slipped disc" on their MRI.
Many people are think that if they have a disc injury, that they'll need surgery to heal it.
However, in most cases, you don't need surgery for a herniated disc.
Spinal discs are commonly described as jelly donuts. The inner layer of the disc is called the nucleus pulposis, and is a soft jelly-like material.
The outer layer is the annulus fibrosis, made of strong collagen fibers.
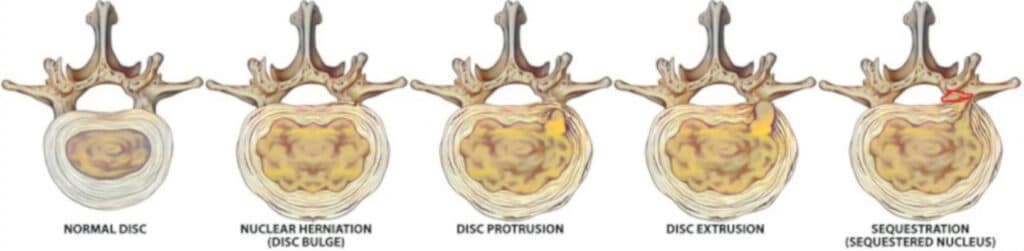
Disc dysfunction on MRI is graded as below:
- Bulging disc - the nucleus pulposis bulges out but not through the annulus fibrosis
- Disc protrusion - the nucleus bulges through the inner wall of the annulus but not all the way through.
- Disc extrusion - the nucleus protrudes all the way through the annulus and extrudes out. This can put pressure on the nerve roots or the spinal cord depending on the side and location.
- Sequestration - a part of the extruded nuclear material breaks off. Often your body can reabsorb this in time.
Disc bulges and protrusions are common. They're present in over 1/3rd of people without symptoms and become more common with age.
Annular fissures (herniated discs) are less common, but they still occur in 20-30% of asymptomatic people.
Should I Worry About The Results Of My MRI Report?
Now that you understand what the terms on your MRI report mean, the next thing you may wonder is if you need to be worried about the findings.
Largely, you don't need to worry about the findings on your MRI report.
Most "abnormal" findings are actually pretty normal features of aging, both in people with and without pain.
Furthermore, only a very small percentage of people with these findings on their MRI actually need surgery.
And interestingly, your conservative treatment (i.e. physical therapy) is largely NOT affected by the findings of your MRI.
In fact, the effect of most conservative treatments for spinal problems don't actually change your anatomy.
Remember, a lot of people without pain have these findings on their MRI report.
YOU might even have had these things before you started having pain.
But usually people only get an MRI after they start having pain, so it's hard to tell whether or not the "abnormal" finding was there before the pain started.
However:
If you have an "abnormal" finding on your MRI and happen to be in pain, there's a good chance that you can get back to a state where you still have that finding on your MRI, but don't have pain.
Surgery is usually only indicated after all of your other conservative treatment options have failed.
Furthermore, back surgery doesn't always work. In fact, after back surgery, 94.0% of people had remaining low back pain, dull ache (71.1%), numbness (69.8%), cold sensations (43.3%), and paresthesia (35.3%) according to a 2017 article in Journal of Pain Research.
What Kind Of Treatment Do I Need?
Getting proper conservative treatment requires an individualized program tailored to meet your specific needs.
At More 4 Life, we often see people who have failed other physical therapy. However, or in-depth evaluation process and personalized 1-on-1 care allows us to help many people who have failed prior physical therapy.
If you need help for neck or back pain and would like to avoid surgery, just tap the button below to request an appointment with one of our specialist physical therapists.