Looking For Chronic Pain Management In St. Louis?
Pain management is nice, but chronic pain relief is better. Our goal is to help you not just "manage" your chronic pain but to find a solution to it so that you can get back to living the life you want.
Watch the video below to learn how we can help you get relief from chronic pain even if others have failed
Need Some Help For Chronic Pain?
Request a Discovery Visit to discover how we can help
Chronic Pain Is Real
If you've lived with chronic pain for months or years or even longer, other people around you may not understand how you feel.
They might even start to imply (or outright say) that you're making it up, that you're crazy, or that it's "all in your head".
But that's just not true.
Chronic Pain Is NOT All In Your Head
On this page, I'll tell you more about the Science of Chronic Pain, but to read more, check out my book:
Chronic Pain, You're Not Just Getting Older, You're Not Crazy, and It's Not All In Your Head

If you'd like MORE help for your Chronic Pain, we'd be happy to help!
Give us a call at 314-941-3970 or tap the button below to request an appointment
The Epidemic of Chronic Pain
Chronic Pain Is Becoming More Common
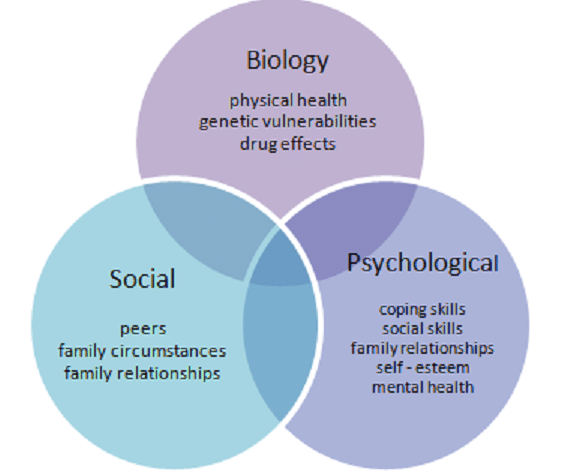
The biopsychosocial model of pain
The International Association for the Study of Pain defines pain as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage.” Note the sensory (the signals our body sends to our brain) and emotional (how our brain interprets those signals) components of the pain are both always present. Our current understanding of pain is that pain is associated with threat. It is protective for our survival. When the brain has more credible evidence of danger than of safety, it produces an unpleasant response (pain) that calls us to take action in order to get out of danger, which we understand as pain. So in summary: danger = pain, safety = no pain. Seems pretty simple…right?
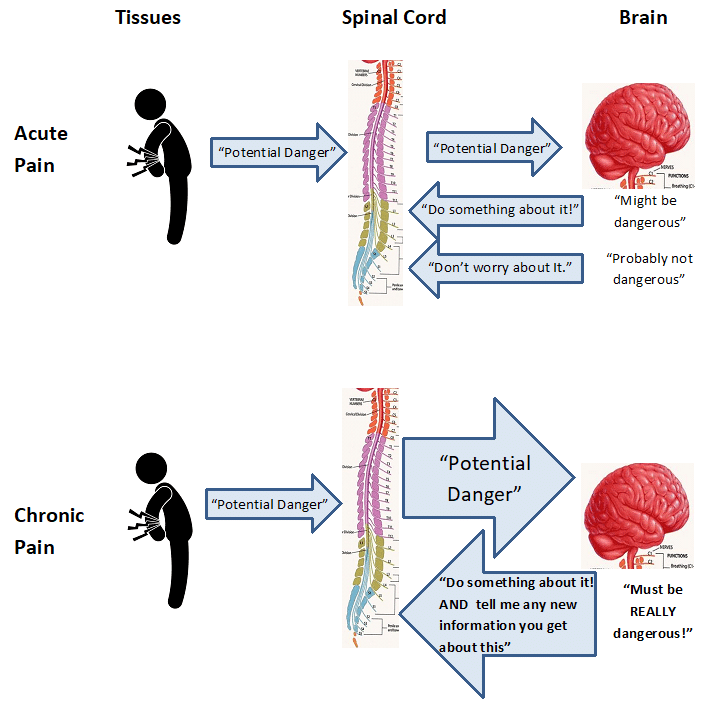
Acute Pain
Acute pain is mostly driven by the sensory signals that come from our body. Imagine for example, if you twisted your ankle. Your brain would send an immediate response to your ankle telling it to get out of that position. You may have some residual signals coming from the tissues due to inflammation, and your brain may tell you to avoid putting weight on the ankle or wear an ankle brace for a few days. The key is that your tissues are sending signals to your brain, your brain is receiving them in proportion to what they should be, and your brain is making appropriate decisions based on that information. This type of pain is adaptive, or beneficial to our well-being.
Chronic or Persistent Pain
Tired of Chronic Pain? Need Some Help?
Request a FREE Phone Consultation with one of our Chronic Pain Experts and get back to doing the things that you need and want to do!